2Department of General Thoracic Surgery, VKF American Hospital, Istanbul, Turkey
3Department of General Thoracic Surgery, Koç University School of Medicine, Istanbul, Turkey
4Department of Pathology, Koç University Hospital, Istanbul, Turkey DOI : 10.26663/cts.2020.00029
Summary
Benign lung tumors are very rare, endobronchial hamartomas -one of which- are even more rare. Endobronchial masses tend to represent themselves via obstruction related symptoms and endobronchial hamartomas are not an exception. It is important to diagnose endobronchial masses before they bring untreatable damage to the lung. It is also important to differentiate endobronchial hamartomas from endobronchial malignancies, such as carcinomas, for they also tend to act mildly symptomatic for a long period of time. In our case, the patient was admitted to our clinic with the symptoms of cough and mild hemoptysis. A computed chest tomography showed total bronchiectasis of right upper lobe along with an endobronchial mass in the right upper lobe bronchus. Bronchoscopic biopsy of the mass revealed no diagnosis. We performed a right upper lobectomy and the pathological examination resulted as endobronchial hamartoma. There are numerous cases about endobronchial hamartomas in the literature which represented with countless symptoms and diseases as persistent cough, recurrent pneumonia, local bronchiectasis and so forth. Our case of endobronchial hamartoma representing with total bronchiectasis of a whole lobe of the lung is the first and only case in the English literature to our knowledge.Introduction
Although lung tumors are predominantly malignant, benign tumors of lung - despite being rare - are clinically important due to their radiological and/or symptomatic presentation. Endobronchial benign tumors are also uncommon and they represent 2% of all lung tumors [1]. Hamartomas are the most common benign tumors of tracheobronchial tree and the lung [2]. They are mostly seen in the peripheral zones of the lung parenchyma. Endobronchial hamartomas are also rare and tend to locate in large bronchi. It may easily be confused with malignant tumors, such as carcinoid tumors. Having said that, endobronchial hamartomas may also cause irreparable lung damage due to obstruction, thus, diagnosis and treatment in the early stages are of vital importance.Case Presentation
A 50-year-old woman was admitted to our clinic for evaluation of persistent cough and mild hemoptysis. A detailed examination of patient’s medical history revealed that the onset of the mentioned symptoms was nearly 10 years prior to admittance. According to the patient’s statement, symptoms have started rather lightly and improved over the years progressively. Cough was persistent, usually non-productive and intensified lately. Hemoptysis has started as blood-tinged sputum and increased seldom, if ever as much as full table spoon. Patient has sought medical help from time to time and had already the diagnosis of bronchiectasis from about 5 years ago. Patient has stated that she visited the hospital irregularly and never received any proper treatment per se. Patient has also stated that she never underwent bronchoscopy or get diagnosed with endobronchial mass. There was no other disease history and the patient was a nonsmoker. A computed tomography (CT) was administered in another hospital before she was admitted, and that CT demonstrated a right upper lobe bronchiectasis along with an endobronchial mass of 0.5 cm (Figure 1).
 Click Here to Zoom |
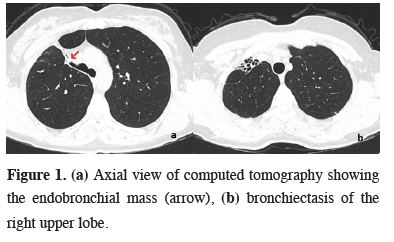
Figure 1: (a) Axial view of computed tomography showing the endobronchial mass (arrow), (b) bronchiectasis of the right upper lobe. |
A fluorodeoxyglucose positron emission tomography (F-18 FDG PET/CT) was also administered at that hospital and it showed a minimally elevated maximum standard uptake volume (SUVmax) as 1.9. Bronchoscopy was performed in our hospital and the endobronchial mass was visualized as a smooth surfaced polypoid body at the entrance of posterior segmental bronchus of right upper lobe, which narrowed the bronchus of right upper lobe. A bronchoscopic biopsy was performed and its pathological examination reported superficial bronchial mucosa, indicating that the biopsy was taken superficially. We performed a video-thoracoscopic right upper lobectomy, since the video-thoracoscopic exploration revealed a totally shrunk right upper lobe and thinned out vasculature of the same lobe in accordance with preoperative CT scan. Another side note of the operation is that the lower and middle lobes were expanded compensatory to fill right hemithorax. An intraoperative frozen section was performed after the lobectomy and it reported the bronchial margins negative and also the endobronchial nodule was in benign nature (Figure 2).
 Click Here to Zoom |
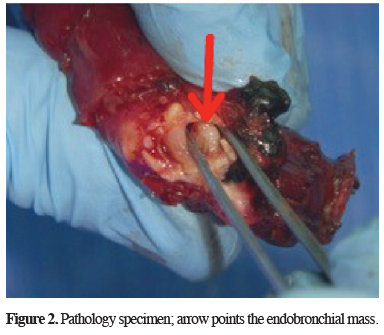
Figure 2: Pathology specimen; arrow points the endobronchial mass. |
Histopathological examination of the specimen revealed the nodule as endobronchial hamartoma (Figure 3).
 Click Here to Zoom |
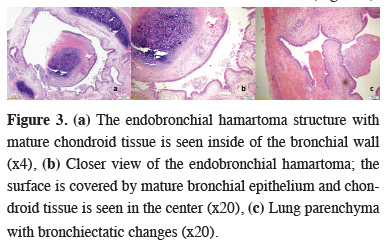
Figure 3: (a) The endobronchial hamartoma structure with mature chondroid tissue is seen inside of the bronchial wall (x4), (b) Closer view of the endobronchial hamartoma; the surface is covered by mature bronchial epithelium and chondroid tissue is seen in the center (x20), (c) Lung parenchyma with bronchiectatic changes (x20). |
Written informed consent was obtained from the patient for publication of her data.
Discussion
Endobronchial hamartomas are predominantly benign tumors and are rare clinical cases. It is important to diagnose endobronchial masses in early stages, before the irreparable lung damage takes place. Obstruction by the endobronchial mass may cause recurrent pneumonia, bronchiectasis, post-obstructive atelectasis, and also malignancies [3].There are various cases in the literature which represented with recurrent pneumonia, persistent cough and even atrial fibrillation along with countless asymptomatic cases [2,4,5]. Some of these cases were reported to be with local bronchiectasis but there is no lobar bronchiectasis in the literature caused by an endobronchial tumor. Due to its nature, lobar bronchiectasis tends to reveal itself as recurrent pneumonia and frequent hospitalization and/or medication history [6]. In spite of our patient have had lobar bronchiectasis, there was no recurrent hospitalization or history of recurrent pneumonia. Nonetheless our patient showed persistent cough and mild hemoptysis, these symptoms does not necessarily indicate bronchiectasis, let alone lobar bronchiectasis.
Hamartomas, including endobronchial ones, incline to stay below-radar in F-18 FDG PET/CT [7,8]. Initial examination and evaluation of all findings, including CT scan and SUVmax value, directed the route towards low activity nodules of the lung: Typical carcinoid, pulmonary adenoma, bronchioloalveolar carcinoma and of course, endobronchial hamartoma [9-11]. There are many options in terms of treatment for endobronchial lesions. Bronchoscopic treatment may be the first one to think as a safe choice: diode laser or argon plasma coagulation and cryotherapy [12]. We have steered for an anatomical resection after a non-diagnostic bronchoscopic biopsy attempt, due to the localization of the mass and bronchiectatic appearance of the right upper lobe in preoperative CT scan. A bronchotomy also comes to mind, but the localization of the mass prevented the idea and also an anatomical resection was already inevitable due to bronchiectasis.
In conclusion endobronchial tumors may cause a variety of symptoms and problems. It is important to detect such masses in early stages, before the irreparable damage takes place. Bronchiectasis, as an irreversible damage entity of the lung, may be the outcome of endobronchial tumors. Our case showed that endobronchial hamartoma caused a total lobar bronchiectasis and is the sole case in the English literature to our knowledge.
Declaration of conflicting interests
The authors declared no conflicts of interest with respect to the authorship and/or publication of this article.
Funding
The authors received no financial support.
Reference
1) Stevic R, Milenkovic B. Tracheobronchial tumors. J Thorac Dis 2016;8:3401-13.
2) Omar AM, Ghanimeh MA, Tylski E, Saettele T. Endobronchial hamartoma: a rare disease with more common presentation. MBJ Case Rep 2016. DOI:10.1136/brj-2016-216771.
3) Prohm P, Winter J, Schmucker P. Pulmonary Hamartoma. Thorac Cardiovasc Surg 1982;30:302-5.
4) Ahmed S, Arshad A, Mador JM. Endobronchial hamartoma; a rare structural cause of chronic cough. Respir Med Case Rep 2017;22:224-7.
5) Schneider F, Winter H, Schwarz F, Niederhagen M, Arias-Herrera V, Martens E et al. Endobronchial Lipomatous Hamartoma: An Incidental 86 Finding in a Patient with Atrial Fibrillation - A Case Report. Case Rep Med 2012. DOI:10.1155/2012/897581.
6) Tsao PC, Lin CY. Clinical spectrum of bronchiectasis in children. Acta Paediatr Taiwan 2002;43:271-5.
7) Jiang L, Huang Y, Tang Q, Zhao Q, Li Y, Wu X et al. 18F‑FDG PET/CT characteristics of pulmonary sclerosing hemangioma vs. pulmonary hamartoma. Oncol Lett 2018;16:660-5.
8) Wang W, Song J, Shi J, Hu H, Wu Y, Yan J et al. Slight uptake of 18F-FDG on positron emission tomography in pulmonary hamartoma: A case report. Oncol Lett 2015;10:430-2.
9) Hochhegger B, Alves GR, Irion KL, Fritscher CC, Fritscher LG, Concatto NH et al. PET/CT imaging in lung cancer: indications and findings. J Bras Pneumol 2015;41:264-74.
10) Moore W, Freiberg E, Bishawi M, Halbreiner MS, Matthews R, Baram D et al. FDG-PET Imaging in Patients With Pulmonary Carcinoid Tumor. Clin Nucl Med 2013;38:501-5.






