

Summary
Background: Blood pleurodesis procedures were generally performed for patients with prolonged air leakage due to pneumothorax. This study investigates the use of blood pleurodesis in patients with prolonged air leak after lung resection and the variables affecting its success.Materials and Methods: A total of 493 patients who underwent anatomical lung resection for nonsmall cell lung cancer between January 2012 and December 2016 were evaluated retrospectively. 68 (13.7%) patients who underwent blood pleurodesis were included the study group. The success rate of the procedure was evaluated according to age, gender, side and type of the surgery, histopathology, and the expansion of the lungs and air leakage.
Results: The success rate was not related to age, sex, side of the operation, histopathology, and type of the resection, while it was found to be statistically significant for the air leakage score (p < 0.001). The procedure was successful in 46 (67.6%) patients and failed in 22 (32.3%) patients.
Conclusions: The blood pleurodesis is a safe, effective and low cost method for treatment of postoperative air leakage in patients with anatomical lung resection for primary lung carcinoma.
Introduction
Prolonged air leakage is a very common complication after lung resection. Air leakage prolongs hospitalisation, increases morbidity and hospital costs. Therefore, many methods have been developed to prevent air leakage. Blood pleurodesis, first performed by Robinson et al. in 1987 [1], has been presented as an ideal method for this purpose with almost no cost and very few complications.Blood pleurodesis procedures described in the literature were generally applied to cases of prolonged air leakage after pneumothorax. Fewer reports have described the use of blood pleurodesis in cases of prolonged air leakage after lung resection.
Blood pleurodesis was shown to effectively resolve prolonged air leakage in studies with few cases, but the factors affecting its efficacy have not been determined. Therefore, the present study was performed to define the factors that affect the results of blood pleurodesis applied between 2012 and 2017.
Methods
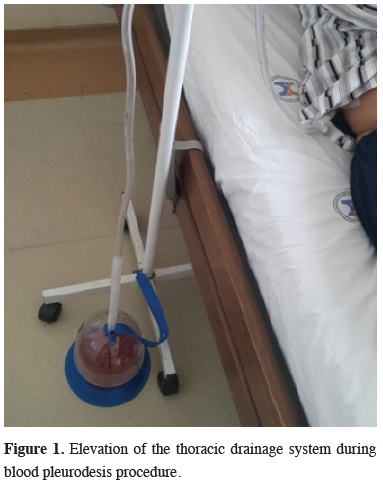
This retrospective study included patients undergoing pulmonary resection and blood pleurodesis due to air leakage between January 2012 and December 2016. The institutional ethics committee approved the study, and all patients provided informed consent. The study population comprised 493 patients aged 18-80 years who underwent anatomical lung resection. Patients undergoing pneumonectomy and non-anatomical lung resection were not included in the study. Those undergoing thoracoscopic lung resection were excluded, whereas those undergoing operations performed with standard posterolateral thoracotomy were included. In the postoperative period, all patients received pulmonary rehabilitation assistance motivation for early mobilisation. Expectorant treatment was included with analgesia. Patients’ chest tubes were connected to suction devices. Patients with persistent air leakage despite these procedures were included in the study. As blood pleurodesis would be meaningless in patients with considerably bloody drainage, patients with bloody drainage were excluded.blood pleurodesis procedure was performed at the bedside in patients with air leakage. Autologous venous blood (100 cc) was taken under aseptic conditions and introduced through the cap-cone connector of the chest drain to prevent coagulation in the tube. To prevent air trapping, the chest drain was hung without being clamped on a serum hanger with a loop, allowing the release of air (Figure 1).
 Click Here to Zoom |
Figure 1: Elevation of the thoracic drainage system during blood pleurodesis procedure. |
No heparin was added to the blood given, but all patients received prophylactic low-molecular-weight heparin (IU/0.4 mL). No sedation or analgesia was required before the procedure. The position of the patient was changed every 30 min, taking special care to manage the drain. The drain was released after 3 h; if air leakage continued, the procedure was repeated the following day. Patients’ chest tubes were removed when air leakage had been resolved. Pleurodesis was deemed successful when patients were discharged with no additional procedure (e.g. pneumoperitoneum, re-thoracotomy, Heimlich valve placement).
Air leakage in the drain was classified as follows [2-4]: 0, no leakage; 1, leakage as 1-2 bubbles during coughing; 2, intense air leakage during coughing; and 3, continuous air leakage during expirium and inspirium.
The success of the procedure was evaluated according to age, sex, side and mode of surgery, malignant/benign differentiation and the degrees of lung expansion and air leakage in the drain.
The required permission was obtained from the patient shown in the figure.
Statistical Analysis
Descriptive statistics were applied to the patients’ demographic and clinical data. The chi-squared test was used to examine correlations between categorical variables, and the Student’s t, Mann–Whitney U and Kruskal–Wallis tests were used for continuous variables. In all analyses, p < 0.05 was taken to indicate statistical significance. SPSS (ver. 22; SPSS Inc., Chicago, IL, USA) was used for the calculations.
Results
Of the 68 patients undergoing blood pleurodesis, 63 and 5 had malignant and benign causes, respectively. The mean age of the patients was 56.9 ± 8.4 (min., 24; max., 78) years. The patients consisted of 61 (89.7%) males and 7 (10.2%) females. Sixteen (23.5%) patients underwent blood pleurodesis on postoperative day 2; the procedure was performed in 14 (20.5%) patients on postoperative day 3, 5 (7.3%) patients on postoperative day 4, 155 (22%) patients on postoperative day 5, 5 (7.3%) patients on postoperative day 6, 6 (8.8%) patients on postoperative day 7, 1 (1.4%) patient on postoperative day 8, 4 (5.8%) patients on postoperative day 9 and 2 (2.9%) patients on postoperative day 10. The mean timing was 5.3 days. The procedure was repeated twice in 22 (32%) patients, three times in 7 (10.2%) patients and four times in 2 (2.9%) patients. Empyema with no reproduction in culture developed in two (2.9%) patients and was controlled by nonspecific antibiotherapy. The procedure was successful in 46 (67.6%) patients and failed in 22 (32.3%) patients.Expansion of the lungs, visualised by posteroanterior chest radiography (PACR), had no significant impact on the procedure (Table 1).
Table 1. The effect of the expansion rate of the lungs on the success of the procedure.
Prolonged air leakage was seen most commonly after right-side surgery, particularly right upper lobectomy (RUL; Table 2).
Table 2. The success of the procedure according to the side and type of the surgery.
However, the rate of successful application did not differ significantly according to the side or type of surgery (Table 3).
Table 3. Surgery type according to the success of the procedure.
The success rate of blood pleurodesis decreased markedly with increasing air leakage score (p < 0.001, Table 4). This rate was not affected by patient age or sex, side of surgery, mode of lobectomy, malignant/benign status, or lung expansion determined by PACR (Table 5).
Table 4. The effect of air leakage score on the success of the procedure.
Table 5. The variables effecting the success rate of the blood pleurodesis procedure.
Discussion
Prolonged air leakage is one of the most frequent complications after lung resection [5-7]. Complications arising from lengthy hospitalisation further prolong hospitalisation and increase costs. New, cost-effective methods to control prolonged air leakage with minimal adverse effects should be investigated.The Heimlich valve, pneumoperitoneum, bronchoscopic valve placement and re-thoracotomy in appropriate patients are more invasive choices that are recommended in cases of prolonged air leakage and are associated with the extension of hospitalisation [5]. Various chemical agents have been used for pleural adhesion in most patients with prolonged air leakage. In general, talc, tetracycline, minocycline, OK-432 (picibanil), povidone-iodine and autologous blood have been used for the treatment of prolonged air leakage in cases of pneumothorax. Blood pleurodesis is used more commonly than these agents because of its significantly reduced adverse effects [8].
Blood pleurodesis was first described by Robinson et al. in 1987 [1] as an alternative to chemical pleurodesis and surgery. It was applied in cases of pneumothorax, and showed a success rate of 85% in a series of 25 patients [1]. In 1992, Dumire et al. [9] first reported the use of blood pleurodesis for prolonged air leakage after resection in a single case; after the failure of tetracycline pleurodesis during 5 weeks of follow-up with a drain, the air leakage ceased after blood pleurodesis. Rivas de Andrés et al. [10] conducted a prospective cohort study of the administration of blood pleurodesis in cases of prolonged air leakage after lung resection. Six patients undergoing surgery for lung cancer and exhibiting prolonged (>10 days) air leakage were followed for a mean of 26.1 months after blood pleurodesis and evaluated. The amount of venous blood used in the procedure was 50-250 cc. The autologous blood was introduced from the end of the chest drain, which was temporarily separated from the water seal. In a letter to the editor, Shackcloth et al. [11] reported on two technical alternatives for this method; they stated that 5, rather than 10, days of air leakage was sufficient to prompt blood pleurodesis, and they recommended the use of a Luer-lock connector instead of separation of the drain from the water seal before the procedure. Drains with cap-cone connectors are used in our clinic, which enable the provision of intra-drain liquid without separation from the water seal.
Decisions about the timing of blood pleurodesis should be made carefully, given the effect of the procedure on the duration of hospitalisation. Cerfolio et al. [2] reported that when postoperative air leakage continues on day 4, the likelihood of its continuance until day 7 is 83%. In such cases, as suggested by Rivas de Andrés et al. [10], it would be more useful to plan blood pleurodesis in the early period instead of waiting for 10 days. However, no consensus on the timing of blood pleurodesis has been established. In the present study, the mean timing for blood pleurodesis was 5.3 days.
In a prospective cohort study performed in 2004, Lang-Lazdunski et al. [12] investigated the effects of blood pleurodesis on prolonged air leakage in 11 patients undergoing surgery for malignant and non-malignant causes. They took a more rigid approach to complications relative to that taken in a prospective cohort study conducted by Çağırıcı et al. [13] with cases of pneumothorax, which yielded the greatest series of adverse effects reported to date. In this study, to prevent bacterial colonisation, 50 cc autologous blood was used, and the drain was clamped after a single pleurodesis procedure. In an editorial published in 2005, Jones et al. [14] stated that patients with air leakage could not tolerate drain clamping and recommended no drain clamping to avoid air trapping, but rather hanging of the drain on the serum hanger with a loop to allow the release of air. With this method, which is preferred in our clinic, the blood remains in the thorax because the drain is higher than the patient’s body and air release is provided because the drain lumen remains open. Clamping of the drain is not recommended in patients with air leakage. Patients with a leakage score of 3 may have temporary air blockage due to clotting in the drain during the blood pleurodesis procedure. Caution is advised in cases in which subcutaneous emphysema and tension pneumothorax may develop. In a prospective randomised study first presented in 2002 and published in 2006, Shackcloth et al. [15] argued that because bacterial colonisation–related complications occurred in cases of prolonged air leakage without blood pleurodesis, these complications could not be related directly to this procedure. Despite the large number of cases included in the present study, empyema with no reproduction in culture developed in only two patients and was controlled by nonspecific antibiotherapy. In a randomised study of 25 patients, Andreetti et al. [16] suggested that 100 cc was more effective than 50 cc autologous blood, in contrast to the results reported by Lang-Lazdunski et al. [12]. Little consensus exists regarding the appropriate amount of blood to use for blood pleurodesis. In our clinic, 100 cc autologous blood is used.
Reports on the use of blood pleurodesis include those by Droghetti et al. [4] (retrospective cohort study, 21 patients), Ahmed et al. [17] (5 patients), and Athanassiadi et al. [18] (prospective cohort study, 20 patients undergoing surgery for malignant/benign causes). Özpolat [19] reported the first application of blood pleurodesis for air leakage developing after hydatid cyst operations.
To our knowledge, this study is among the largest (with 68 patients) to examine the experience with blood pleurodesis in patients with prolonged air leakage after lung resection. The success rate of the procedure was 67.6%, similar to previous reports [15,20-22]. The main limitations of this study include its retrospective design and the lack of a control group for comparison.
The mechanism of spontaneous regression of air leakage after lung resection is not clear. However, it is likely due to the closure of minimal tears in the visceral pleura following visceral-parietal apposition and adhesion [5]. Blood pleurodesis has two effects on air leakage [1,9]. The ‘patch’ effect, in which venous blood introduced into the thorax prevents air leakage by covering lacerations on the visceral pleura, is the most important. This mechanical effect is effective for early air leakage and is in fact not pleurodesis. Although it does not correspond to the nomenclature, this ‘patch’ effect of blood pleurodesis is a unique feature that cannot be obtained with chemical pleurodesis agents. The second, i.e. ‘desis’, effect of blood pleurodesis involves adhesion in the pleural leaves due to the long-term organisation of the introduced blood. Although some authors have recommended the opposite [23], the clinician does not need to wait for the lung to be fully expanded before performing blood pleurodesis. Indeed, lung expansion had no significant effect on the efficiency of the procedure in the present study. In our clinic, low-molecular-weight heparin is administered subcutaneously to all patients postoperatively for prophylaxis. No adverse effect of prophylactic heparin on the success of blood pleurodesis has been reported [12].
In the present study, procedures on the right side, especially RUL, more commonly led to the requirement for blood pleurodesis. The risk of postoperative air leakage is higher following upper lobectomy because the potential air space remaining in the apical area prevents pleural apposition and adhesion [2,24,25]. Approximately 25% of cases of prolonged air leakage develop after upper lobectomies, and this leakage is the sole complication in 81% of these cases [6]. Emphysema, chronic obstructive pulmonary disease and incomplete fissure are also responsible for postoperative prolonged air leakage [2,5,6,25,26]. On the other hand, in the present study, the effects of the level and side of lobectomy on the efficiency of blood pleurodesis were not significant, and the pleural approach may not be necessary for blood pleurodesis due to the ‘patch’ effect.
In the present study, factors such as age, sex and cause of resection (malignant/benign) did not influence the success of pleurodesis, but the success rate decreased with increasing air leakage score (p < 0.001). As air trapping may cause tension pneumothorax in patients with severe air leakage, the performance of blood pleurodesis with two chest drains in these patients is safer.
Several methods are available for the treatment of air leakage, including prolonged tube thoracostomy, chemical pleurodesis and surgical repair, but little consensus has been achieved on the role and timing of blood pleurodesis. Several prospective studies showed that autologous blood pleurodesis has superior outcomes in cases of persistent air leakage in terms of success rate, sealing time and complication rates in comparison with conservative treatment without opposition. No unpredictable reaction that may develop with the application of talc, the most common pleurodesis agent, was seen in patients undergoing blood pleurodesis in the present study. In cases requiring re-thoracotomy and in which blood pleurodesis was not effective, blood pleurodesis caused less inflammation than talc pleurodesis and allowed dissection because it did not cause intense adhesions. Therefore, blood pleurodesis is superior to talc pleurodesis.
New products, such as patches, glues and sealants, are currently being developed to help treat air leakage in the operation room. However, some of these products are expensive and their application requires special equipment. Here, we suggest a simple and inexpensive procedure that is available to all thoracic surgeons to help manage air leakage postoperatively. This method should at least be tried, even in patients for whom definite success is not expected.
As a conclusion, blood pleurodesis is a simple, safe, painless, effective and low-cost treatment for postoperative air leakage in patients who have undergone anatomical lung resection for primary lung carcinoma. The main advantages of the procedure are the use of the patient’s own blood and the lack of requirement for additional equipment. It can also be applied in cases in which lung expansion has not been achieved.
Declaration of conflicting interests
The authors declared no conflicts of interest with respect to the authorship and/or publication of this article.
Funding
The authors received no financial support.
Reference
1) Robinson CL. Autologous blood for pleurodesis in recurrent and chronic spontaneous pneumothorax. Can J Surg 1987; 30: 428-9.
2) Cerfolio RJ, Tummala RP, Holman WL, Zorn GL, Kirklin JK, McGiffin DC, et al. A Prospective Algorithm for the Management of Air Leaks After Pulmonary Resection. Ann Thorac Surg 1998; 66: 1726-31.
3) Cao Gq, Kang J, Wang F, Wang H. Intrapleural Instillation of Autologous Blood for Persistent Air Leak in Spontaneous Pneumothorax in Patients With Advanced Chronic Obstructive Pulmonary Disease. Ann Thorac Surg 2012; 93: 1652-7.
4) Droghetti A, Schiavini A, Muriana P, Comel A, De Donno G, Beccaria M. Autologous blood patch in persistent air leaks after pulmonary resection. J Thorac Cardiovasc Surg 2006; 132: 556-9.
5) Venuta F, Rendina EA,De Giacomo T, Coloni GF. Postoperative Strategies to Treat Permanent Air Leaks. Thorac Surg Clin 2010; 20: 391-7.
6) Abolhoda A, Liu D, Brooks A, Burt M. Prolonged air leak following radical upper lobectomy: an analysis of incidence and possible risk factors. Chest 1998; 113:1507-10.
7) Okereke I, Murthy SC, Alster JM, Blackstone EH, Rice TW. Characterization and importance of air leak after lobectomy. Ann Thorac Surg 2005; 79: 1167-73.
8) How CH, Hsu HH, Chen JS. Chemical pleurodesis for spontaneous pneumothorax. J Formos Med Assoc 2013; 112: 749-55.
9) Dumire R, Crabbe MM, Mappin FG, Fontenelle LJ. Autologous ‘bloodpatch’ pleurodes is for persistent pulmonary air leak. Chest 1992; 101: 64-6.
10) Rivas de Andrés JJ, Blanco S, de la Torre M. Post surgical pleurodesis with autologous blood in patients with persistent air leak. Ann Thorac Surg 2000; 70: 270-2.
11) Shackcloth MJ. Autologous blood pleurodesis for treating persistent air leak after lung resection. Ann Thorac Surg 2001; 71: 1402-3.
12) Lang-Lazdunski L, Coonar AS. A prospective study of autologous ‘bloodpatch’ pleurodesis for persistent air leak after pulmonary resection. Eur J Cardiothorac Surg 2004; 26: 897-900.
13) Cagirici U, Sahin B, Cakan A, Kayabas H, Buduneli T. Autologous blood patch pleurodesis in spontaneous pneumothorax with persistent air leak. Scand Cardiovasc J 1998; 32: 75-8.
14) Jones NC, Curry P, Kirk AJB. An alternative to drain clamping for blood pleurodesis. Eur J Thorac Cardiovasc Surg 2005; 27:935.
15) Shackcloth MJ, Poullis M, Jackson M, Soorae A, Page RD. Intrapleural instillation of autologous blood in thetreatment of prolonged air leak after lobectomy: a prospective randomized controlled trial. Ann Thorac Surg 2006; 82: 1052-6.
16) Andreetti C, Venuta F, Anile M, De Giacomo T, Diso D, DiStasio M. Pleurodesis with an autologous blood patch to prevent persistent air leaks after lobectomy. J Thorac Cardiovasc Surg 2007; 133: 759-62.
17) Ahmed A, Page RD. The utility of intrapleural instillation of autologous blood for prolonged air leak after lobectomy. Curr Op in Pulm Med 2008; 14: 343-7.
18) Athanassiadi K, Bagaev E, Haverich A. Autologous blood pleurodesis for persistent air leak. Thorac Cardiovasc Surg 2009; 57: 476-79.
19) Ozpolat B. Autologous blood patch pleurodesis in the management of prolonged air leak. Thorac Cardiovasc Surg 2010; 58: 52-4.
20) Rinaldi S, Felton T, Bentley A. Blood pleurodesis for the medical management of pneumothorax. Thorax 2009; 64: 258-60.
21) Cobanoğlu U, Melek M, Edirne Y. Autologous blood pleurodesis: a good choice in patients with persistent air leak. Ann Thorac Med 2009; 4: 182-6.
22) Karangelis D, Tagarakis GI, Daskalopopoulos M, Skoumis G, Desimonas N, Saleptsis V, et al. Intrapleural instillation of autologous blood for persistent air leak in spontaneous pneumothorax- is it as effective as it is safe? J Cardiothorac Surg 2010; 5: 61.
23) Ando M, Yamamoto M, Kitagawa C, Kumazawa A, Sato M, Shima K. Autologous blood-patch pleurodesis for secondary spontaneous pneumothorax with persistent air leak. Respir Med 1999; 93: 432-4.
24) Miller JL Jr. Acute and delayed space problems following pulmonary resection. Chest Surg Clin North Am 1996; 6: 615-21.



