2Department of Thoracic Surgery, Medicana International Hospital, Ankara, Turkey
3Department of Pathology, Gazi University School of Medicine, Ankara, Turkey
4Department of Thoracic Surgery, Gazi University School of Medicine, Ankara, Turkey DOI : 10.26663/cts.2019.00019
Summary
A 33-year-old male patient was complaining about shoulder pain and swelling in his neck. The computed tomography of the patient revealed a mass lesion extending from the supraclavicular region to the upper level of the aortic arch. The patient was operated with the Grunenwald incision approaching from the anterior. The mass was separated from the tissues and totally excised. The histopathological examination reported a biphasic synovial sarcoma. Here we evaluated a very rare case of primary synovial sarcoma in the context of the literature, localized at the thoracic inlet and excised by the Grunenwald incision.Introduction
Soft tissue sarcomas are rarely seen connective tissue tumors. Synovial sarcomas (SS) constitute 5-10% of the soft tissue sarcomas. They are mostly localized at the lower extremities at a rate of 65%, but they can also localized in thorax in rare cases [1]. Since they are aggressive tumors, surgery becomes the major approach in their treatment.Here, we presented a very rare case of primary synovial sarcoma localized at the thoracic inlet, which was excised by way of the Grunenwald incision.
Case Presentation
A 33-year-old male patient presented to our clinic complaining about shoulder pain and swelling in his neck. The computed tomography (CT) of the thorax revealed a mass lesion of 82x68 mm extending from the supraclavicular region to the upper level of the aortic arch invading left subclavian artery and scalene muscles (Figure 1). Positron emission tomography revealed a SUVmax value as 5.8. As the pathologic examination of the transthoracic tru-cut biopsy demonstrated Ewing sarcoma, he received six cycles of cisplatin and etoposide chemotherapy. Seeing that there was no regression in the mass and the patient’s shoulder pain increased after chemotherapy. Since the patient did not accept the additional treatment after the chemotherapy, the decision for surgical treatment was taken by the oncology council.
 Click Here to Zoom |
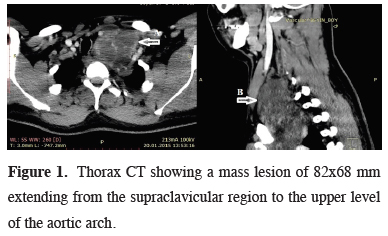
Figure 1: Thorax CT showing a mass lesion of 82x68 mm extending from the supraclavicular region to the upper level of the aortic arch. |
The patient was scheduled for surgery. The Grunenwald incision was performed with an anterior approach (Figure 2).
 Click Here to Zoom |
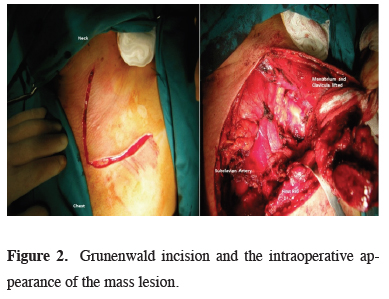
Figure 2: Grunenwald incision and the intraoperative appearance of the mass lesion. |
In the exploration, a cystic mass was found tightly adhered the vascular-nerve bundle at the medial, left subclavian artery at the inferior, and brachial plexus, phrenic nerve and scalene muscle at the base. The mass was separated from the surrounding tissues. Wedge resection was performed to the area subject to the invasion in the apicoposterior segment of the upper lobe of the lung ensuring for R0 resection. The postoperative pathology of the patient was reported as biphasic synovial sarcoma (Figure 3). The patient is still being followed up by oncology in his postoperative 2nd year. There were no metastases detected.
 Click Here to Zoom |
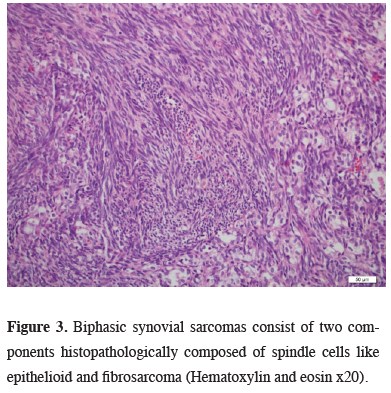
Figure 3: Biphasic synovial sarcomas consist of two components histopathologically composed of spindle cells like epithelioid and fibrosarcoma (Hematoxylin and eosin x20). |
Discussion
Synovial sarcomas (SS) are soft tissue tumors typically occurring in adolescents and young adults (between 15 and 40 years of age) and showing mesenchymal and connective tissue differentiation [1]. They usually involve the larger joints of the extremities. They are rarely localized in the neck, tongue, larynx, heart, esophagus, lungs and mediastinum. 74-81% of them may cause lung metastasis [2]. An SS primarily originated from the lungs was first published by Zeren et al [3]. In our case, it was originated from the thoracic inlet. This localization has been described in the literature very rarely [4,5]. A case where surgical resection could be carried out in this region was not encountered in the English literature.Patients mostly complain about chest pain. There may also be other complaints including a cough, shortness of breath and hemoptysis [2]. In our case, the patient had severe shoulder pain and swelling in the neck because the tumor was close to the brachial plexus. Lung cancer (superior sulcus tumors), neurogenic and malignant triton tumors should be kept in mind in the differential diagnosis of the thoracic inlet masses.
SS are less chemoradiosensitive tumors compared to Ewing sarcomas. The rate at which they respond to chemotherapy ranges between 28-47% in the publications [6,7]. Fluorescence in situ hybridization analysis identification of the diagnostic chromosomal translocation (t[X;18][p11.2;q11.2]), a marker for this tumor, resulting from fusion of the SYT gene on chromosome 18 to either the SSX1 or SSX2 gene on chromosome X was the most reliable diagnostic method [4,8].
Thoracic inlet tumors are challenging operations for thoracic surgeons due to major vascular and nerve structures. Dartavelle uses an L-shaped incision extended from the anterior of the sternocleidomastoid muscle to the intercostal area, and clavicle and manubrium resection are required [5] In literature, this incision is often preferred for anterior Pancoast tumors [6]. Rarely this technique has been described for subclavian artery aneurysms and sarcomas. The conventional thoracotomy incisions are not sufficient for resection in thoracic inlet tumors. In such cases, the Grunenwald incision enables easy access to thoracic inlet tumors. Unlike the Dartevelle technique, the clavicle is protected in this technique [7]. Both techniques were better defined in terms of patient comfort compared to thoracotomy. Since the patient did not accept the additional treatment after the chemotherapy, the decision was taken by the oncology council for surgery. We also preferred an anterior approach in our patient both to detach the tumor from around the brachial plexus and to reach the apical area of the lung. Furthermore, adverse effects on chest wall mechanics well established after thoracotomy have not been observed with the Grunenwald approach.
In conclusion, primary synovial sarcoma has a poorer prognosis compared to other types of sarcomas. Excision should first be considered as the main treatment in these patients. In particular, the Grunenwald incision is an appropriate approach to better control the thoracic inlet anatomy.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Reference
1) Weiss SW, Goldblum JR. Fibromatoses. In: Weiss SW, Goldblum JR, editors. Enzinger and Weiss’s soft tissue tumors. 4th ed. St Louis: Mosby; 2001. pp. 309-46.
2) Spurrell EL, Fisher C, Thomas JM, Judson IR. Prognostic factors in advanced synovial sarcoma: an analysis of 104 patients treated at the Royal Marsden Hospital. Ann Oncol 2005; 16: 437-44.
3) Zeren H, Moran CA, Suster S, Fishback NF, Koss MN. Primary pulmonary sarcomas with features of monophasic synovial sarcoma: a clinicopathological, immunohistochemical, and ultrastructural study of 25 cases. Hum Pathol 1995; 26: 474-80.
4) Galetta D, Pelosi G, Leo F, Solli P, Veronesi G, Curto B Del, et al. Primary thoracic synovial sarcoma: Factors affecting long-term survival. J Thorac Cardiovasc Surg 2007; 134; 808-9.
5) Mirza AK, Barrett IJ, Rathore A, Bassem T, Rose PS, Shives T, et al. Soft tissue neoplasms causing apparent venous thoracic outlet syndrome. Ann Vasc Surg 2017; 42: 306.e1-306.e4.
6) El L, Sp J, Bl H, Cesne A Le, Ouali M, Leahy MG, et al. Doxorubicin-based adjuvant chemotherapy in soft tissue sarcoma : pooled analysis of two STBSG-EORTC phase III clinical trials. Ann Oncol 2014; 25: 2425-32.






