

2Department of Thoracic Surgery, Istinye University Medical Faculty, Liv Hospital Ulus, Istanbul, Turkey
3Department of Thoracic Surgery, University of Health Sciences, Yedikule Chest Diseases and Thoracic Surgery Education and Research Center, Istanbul, Turkey
4Department of Thoracic Surgery, Bezmialem Vakif University, Istanbul, Turkey DOI : 10.26663/cts.2020.0001
Summary
Background: Pulmonary artery reconstruction can be preferred as an alternative to pneumonectomy, to spare the functional lung parenchyma in lung cancer. This study aimed to evaluate the morbidity, mortality and survival rates of the patients who had undergone pulmonary artery reconstruction due to central non-small cell lung cancer (NSCLC) and also to compare their data with those of the patients who had undergone pneumonectomy.Materials and Methods: In this study, 88 patients who underwent pneumonectomy (group PN) and 20 patients who underwent standard or sleeve lobectomy (double sleeve) with pulmonary artery reconstruction (group PAR) for NSCLC with stages I-IIIA between January 2005 and December 2010 were evaluated retrospectively. The morbidity and mortality rates, durations of the hospital and intensive care unit stay, 5-year and mean survival rates of the homogenous patient groups were analyzed comparatively.
Results: The postoperative morbidity rate was 30% in the PAR group and 53% in the PN group (p = 0.77). The bronchial complication rate was 0% in the PAR group and 15% in the PN group (p = 0.04). The 30-day mortality rate was 5% in the PAR group and 5.6% in the PN group (p = 1). The median follow-up period for all patients was 31.5 months (range: 0-84 months) and total 5-year survival was 56.2%. In early-stage tumors (stage I + stage II), total 5-year survival rate was 64% in the PAR group and 60% in the PN group (p = 0.7). In late-stage tumors (stage III), total 5-year survival rate was 52% in the PAR group and 30% in the PN group (p = 0.04). No local recurrence was observed in either group during the follow-up period.
Conclusions: In central lung tumors, to avoid pneumonectomy, major anatomical lung resection with pulmonary artery reconstructions can safely be performed with acceptable morbidity and mortality rates. Oncological outcomes of pulmonary angioplasty procedures regarding survival and local recurrence are not worse than those of pneumonectomy. Even in advanced stage lung tumors, these procedures can be an alternative to more radical operations such as pneumonectomy.
Introduction
Pneumonectomy has been performed as a standard surgical method in the curative treatment of patients with central lung tumors for decades, [1]. The limited physiological reserve after pneumonectomy (PN) is considered to cause higher morbidity and mortality than lobectomy [2-6]. Since the sparing of functional lung parenchyma provides a higher quality of life, bronchial sleeve resections have been used as an alternative to pneumonectomy in central lung tumors [7,8]. In many comparative publications up to date, the perioperative risk of bronchial sleeve resection is shown to be comparable to that of standard lobectomy [9-11], and it has been noted that its long-term survival outcomes and tumor recurrences are similar to or better than pneumonectomy [10,12,13]. Knowing that pneumonectomy alone is a mortality-increasing operation, it has recently been reported that independent of pulmonary functions, parenchyma sparing surgeries (PSS) are also widely performed in patients who can tolerate pneumonectomy [1,14].The only alternative to pneumonectomy is pulmonary artery reconstruction (PAR) combined with lobectomy or bronchoplasty if there is main pulmonary artery involvement in the central pulmonary tumors, [15]. Although high mortality and morbidity rates have been reported in the early reports of this parenchyma sparing lung resection [16], the advantages of pulmonary angioplastic procedures have been shown in recent studies [17-20], and thus these applications have become increasingly popular in lung cancer surgery. Especially, the increase in the long-term satisfactory results of the bronchovascular sleeve resections [1,15,17,18,20-23] has been the basis of pulmonary angioplasties performed to avoid pneumonectomy in central lung tumor patients with pulmonary artery invasion. However, in the literature, there are only a few clinical studies comparing pneumonectomy performed with angioplasty procedures in terms of operative mortality, morbidity, survival and recurrence rates [1,21,24-27]. In these studies, PAR has generally been applied to heterogeneous patient populations with different surgical techniques for different indications, and it has been considered as a variation of bronchoplastic procedures (extended sleeve) when comparing its results with the results of the patients who underwent PN; therefore, it is difficult to make a precise interpretation about the superiority of PAR itself to PN.
This retrospective study aims to investigate the patients who underwent pulmonary artery reconstruction due to central non-small cell lung cancer (NSCLC) with pulmonary artery involvement in terms of morbidity, mortality and survival rates and to compare these results with the results of the patients who underwent pneumonectomy in the same period.
Methods
All of the patients who were treated in our clinic gave informed consent by signing a statement allowing the use of their data for clinical trials. The study was approved by the institutional review board (2019-004-002) and was conducted in accordance with the principles of the Declaration of Helsinki.
Patient Criteria
In the study; six hundred and thirty-six patients who were diagnosed with NSCLC, ranging from stage I to III A, and underwent lung resection in Yedikule Chest Diseases and Thoracic Surgery Education and Research Hospital between January 2005 and December 2010 were analyzed. Among these, a total of 139 patients were studied retrospectively, of whom 22 had undergone pulmonary artery reconstruction, and 117 had undergone pneumonectomy. Data collection for analysis was ended in November 2012.
Tangential resection and primary suturation of the pulmonary artery (PA), patients with simple closure of a single PA branch or PA damage repair, patients who received neoadjuvant therapy, patients with ‘T4’ tumor, patients who had ‘N2’ lymph node metastasis or R1 microscopic residual disease, patients who underwent extended resection such as chest wall resection or carina resection, carcinoid tumors, lung tumors with the brain and surrenal metastasis, patients who were operated for recurrent lung tumors and completion pneumonectomy were excluded from the study for the sake of homogeneity between the groups. In conclusion, 20 patients (group PAR) who underwent pulmonary artery reconstruction and 88 patients (group PN) who underwent pneumonectomy in the same period were included in the study.
Preoperative Preparation
All patients underwent the standardized diagnostic and staging procedures preoperatively. Histopathological diagnostic specimens were obtained by either fiberoptic bronchoscopy or computed tomography (CT)-guided needle biopsy. CT scans of each patient’s chest and upper abdomen, bone scintigraphy, and brain magnetic resonance imaging (MRI) or Positron-emission tomography (PET) study were performed for noninvasive staging. Each patient also underwent a pulmonary function test, electrocardiography, and arterial blood gas analysis to evaluate the operative risk. Pulmonary angiography was performed in selected cases to evaluate the degree of pulmonary artery invasion. All patients suspected of having N2-N3 lymph node metastasis underwent cervical mediastinoscopy-mediastinotomy-extended mediastinoscopy.
Surgical Method
Single-lung ventilation was established through a double-lumen endotracheal tube. A routine posterolateral thoracotomy in the fifth intercostal space was performed. Mediastinal and hilar lymph node dissection was routinely performed, and frozen sections were studied. Patients who had a central tumor in the entrance of lobar bronchus and who had positive surgical margin after standard lobectomy underwent bronchoplastic procedure in which end-to-end style anastomosis was performed using a continuous suturing technique with 3-0 non-absorbable material (Prolene Ethicon Inc, Hamburg, Germany). Where safe dissection of pulmonary artery branches was not possible due to tumor invasion, but complete surgical resection with standard or sleeve lobectomy could be achieved, patients underwent PA resection and reconstruction procedures to avoid pneumonectomy. After the resection of the tumor-effected part of the PA, bronchus was also resected, and the tumor-bearing lobe was removed en-block. Meanwhile, frozen section examinations were performed both for the bronchus and for the resected part of the PA to be sure that there was no tumor at the margins of the resection.
At the pulmonary artery reconstruction phase, patch angioplasty was performed if PA diameter was resected up to the half; if more than half of the PA diameter was resected, sleeve angioplasty (sleeve resection and end-to-end anastomosis) was performed. In all patients who underwent patch angioplasty, the autologous pericardium removed from the anterior part of the phrenic nerve was used for patching. The graft was patched using continuous suture technique with 5-0 monofilament non- absorbable material (Prolene Ethicon Inc, Hamburg, Germany). If a concomitant bronchoplastic procedure would also be performed, patch angioplasty was performed before the bronchial anastomosis to reduce the clamping time of the pulmonary artery. In sleeve angioplasty requiring patients, PA anastomosis was performed after the bronchial anastomosis to minimize vascular manipulation and to shorten the distance between the distal and proximal edges to decrease the tension. Pulmonary artery anastomosis was performed using a continuous suture technique with 5-0 monofilament non-absorbable material (Prolene Ethicon Inc, Hamburg, Germany). In double sleeve performed patients, pedicled pericardium or pleural flap was interposed between the tissues of the anastomosis. In the pneumonectomy group, closure of the main bronchus after resection was performed with two or four rows of 3-0 non-absorbable suture (Prolene Ethicon Inc, Hamburg, Germany). All patients included in the study were extubated on the operation room and were transferred to the intensive care unit.
Postoperative Period
Fiberoptic bronchoscopy was performed in the postoperative period if the patient developed secretion retention or if any anastomotic complications were suspected. In PAR group, long-term oral anticoagulation was not considered necessary in patients who underwent patch angioplasty. However, patients who underwent sleeve angioplasty received IV heparin during hospitalization and oral anticoagulant for 3 months following discharge to prevent clot formation due to anastomotic turbulence.
Postoperative histopathological staging (pTNM) was performed. The resected specimen was examined histopathologically and the histologic type was determined according to the WHO classification [28]. Surgical pathological staging was performed according to the 7th TNM grading system adopted by the American Joint Committee for Cancer (AJCC) in 2009 [29]. Routine postoperative follow-up included an office visit with a physical examination, serial chest radiographs, and computed tomography every 3-6 months.
Postoperative complications, days of postoperative stay in intensive care, and postoperative hospitalization were considered as morbidity indications [24]. The development of any fatal complications within the postoperative 30 days or death before discharge was defined as postoperative mortality. The day the patient underwent operation was taken base for the survival analysis, and the calculation was made according to it. Any tumor or mediastinal lymph node development having the same histology as the original tumor in the resected hemithorax was defined as the local recurrence of the disease.
Statistical Analysis
Demographic data, morbidity and mortality rates were calculated as percentages and compared using the X2 or Fisher’s Exact test. Kaplan-Meier survival analysis was used for survival and Mann Whitney U test for continuous variables. P-value of less than 0.05 was considered to be statistically significant. SPSS 10.0 packaged software was used for analysis.
Results
1. Characteristic FeaturesSimilar general characteristics of patients are given in Table 1.
Table 1: Clinical and pathological features of the patients.
Although both groups underwent left-dominant operations, this dominance was statistically significant in PAR group (p = 0.04). Types of concomitant resections and angioplasties performed on the patients in PAR group (n = 20) are given in Table 2.
Table 2: Types of concomitant resections and angioplasties performed in PAR group.
Together with pulmonary angioplasty, nine patients underwent standard lobectomy (left upper lobectomy, n=7; right upper lobectomy, n=1; right lower lobectomy, n=1), eleven underwent sleeve lobectomy (left sleeve upper lobectomy, n=10; right sleeve upper bilobectomy, n = 1). In all patients who underwent double sleeve lobectomy, a left-sided procedure was performed. All patients underwent PAR due to direct tumor invasion. Of the thirty-four right pneumonectomies, five were intrapericardial (14%); of the fifty-four left pneumonectomies, nine were intrapericardial (16%). Of the patients, fifty-six underwent pneumonectomy due to fissure invasion, 12 (left pneumonectomy, n = 8; right pneumonectomy, n = 4) due to vascular invasion, and 20 due to main bronchial tumor.
2. Morbidity Indications
Postoperative complications used as indications of morbidity were evaluated, and they were summarized in Table 3.
Table 3: Peroperative complications as indicators of mor-bidity.
In the PAR group, 13 complications (8 minor, 5 major) developed in six patients and the morbidity rate was 30%. In the PN group, 81 complications (30 minor, 51 major) were observed in forty-seven patients and the morbidity rate was 53%. When groups were compared, there was no significant difference in morbidity rates (p = 0.77), although, more patients in the PN group had more complications.
The most frequent complications in both groups were pulmonary complications. The most common cause of pulmonary complications in both groups (group PAR, n = 4; group PN, n = 23) was secretion retention/ atelectasis requiring FOB or nasotracheal aspiration (NTA). No significant difference was observed between the groups in terms of therapeutic FOB requirements (p = 0.32).
No bronchial dehiscence or late-term non-neoplastic stricture development was observed in PAR group patients, while in the PN group 14 (15%) patients developed a broncho-pleural fistula. Of the patients with fistula, 10 underwent right PN and 4 left PN. A significant difference observed between the groups in terms of bronchopleural fistula development (p = 0.04).
Pleural drainage and irrigation were performed on 14 patients who developed BPF in the PN group; via thoracostoma in seven and tube thoracostomy in 3. Two patients underwent stump revision and omentoplasty, and of the remaining 2; 1 underwent sternotomy with bronchial occlusion in the early period, and the other underwent endobronchial closure with FOB.
No significant difference was observed between the hospital stays of the patients in PAR and PN groups (Table 4) (p = 0.38). Intensive care unit stay was 2.9 ± 7.8 days (min: 1-max: 36) in the PAR group and 2.4 ± 6.8 days (min: 1-max: 60) in the PN group. There was no significant difference between the groups in terms of intensive care unit stay (p = 0.80). Since all patients were followed up in the intensive care unit on the postoperative 1st day, the patients were also studied for the ratio of the patients who stayed for 1 day and those who stayed for longer than 1 day, and no statistically significant difference was observed between the two groups (Table 4) (p = 0.82).
Table 4: Hospital stay and ICU stay as indicators of mor-bidity.
3. Mortality
In the PAR group, in one patient who could not be extubated in the postoperative period, hospital mortality occurred due to ventilator-associated pneumonia, ARDS, sepsis and multi-organ failure on the 28th day (5%). In the PN group, hospital mortality occurred in 5 patients (%5.6). Of these 5 hospital mortalities; 2 occurred on the 19th and 21st days due to sepsis and multi-organ failure following post-operative pneumonia, 1 occurred due to bronchopleural fistula and empyema on the 12th day, and the other 2 occurred due to cardiac and renal problems on the 16th and 24th days. When the groups were evaluated in terms of mortality rates; although there was a higher rate of mortality in PN group, no significant difference was determined (p > 0.05) (Table 5).
Table 5: Postoperative mortality.
4. Survival
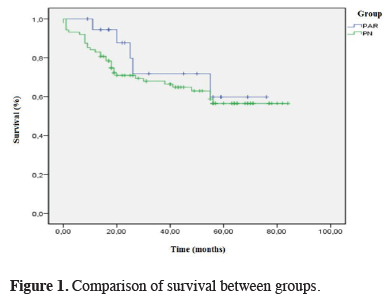
The median follow-up period for all patients was 31.5 months (range: 0-84 months) and total 5-year survival was 56.2%. In November 2012, when the follow-up was terminated, 13 (65%) patients in the PAR group and 55 (62%) in the PN group were alive. The two groups were similar in terms of follow-up periods (p = 0.75). Overall 5-year survival results (59.8% and 56%, respectively) and mean survival time (58 and 54 months, respectively) were more advantageous in the PAR group compared to the PN group (p = 0.81); however, this advantage was not statistically significant (Figure 1).
 Click Here to Zoom |
Figure 1: Comparison of survival between groups. |
While total 5-year survival rates were similar in both groups in early-stage (stage I + II) tumors (p = 0.73), total 5-year survival in late-stage (stage III) tumors was observed to be significantly better in the PAR group (p = 0.04).
Discussion
If any cure could be offered for lung cancer, surgical resection is the most important treatment method today. Complete resection is associated with tumor recurrence and survival, and the amount of resected pulmonary tissue is associated with perioperative morbidity, mortality and quality of life [4,27,28].Since pneumonectomy has high mortality and morbidity and decreases the patient’s quality of life, parenchyma sparing bronchoplastic and angioplasty procedures have been defined [29,30]. If the tumor has invaded the pulmonary artery, the only alternative to pneumonectomy is the reconstruction of PA, no matter bronchoplasty is required or not. However, based on the results of the early publishments, this technique was thought to be laborious, time-consuming and associated with high mortality and morbidity rates [31]. Until Rendina et al. [17,32] had published many specific intraoperative techniques related to PA sleeve resection and their positive results, difficulties were encountered in the acceptance of PA reconstruction, and no real advance could be achieved. Furthermore, there were serious concerns about the probability of a high tumor recurrence risk, which would limit survival [33], and this technique was not adopted by many thoracic surgeons.
Due to the recently reported acceptable morbidity, mortality and long-term survival outcomes of PA resection and reconstruction concurrent with lobectomy, this technique has been accepted as an advantageous alternative to pneumonectomy [1,17,18,21,34]. In our study, the morbidity rates observed in PAR and PN groups were 30% and 53%, respectively. No significant difference was observed between the groups in terms of the incidence of morbidity. However, when bronchial morbidities were taken into consideration, statistically significantly higher BPF was identified in the PN group (p = 0.04). This showed us that in central lung tumors, pulmonary artery reconstruction concurrent with standard or sleeve lobectomy could be employed with lower peroperative risk compared to pneumonectomy.
In PAR group, no procedure-specific mortal complications such as dehiscence on the bronchial or vascular anastomosis site or broncho-vascular fistula were observed. It demonstrated the importance of covering the anastomosis site with living tissues such as the pleural or intercostal muscle flap, just as we did in our cases. In particular, it emphasized that the intercostal muscle flap prevents the development of bronchopleural fistula by providing airway continuity even if small dehiscences may occur in the anastomosis site. It has also been reported in the literature that many materials such as pericardium, pericardial fatty tissue, omentum, mediastinal pleura and azygos vein can be used for covering [22,24,26,34]. Besides, PA thrombosis is quite a rare complication [20,32], as supported by the literature, and should not be a concern about PAR. In our study, too, no symptoms of PA thrombosis or occlusion was observed in, and follow-up contrast-enhanced thorax CT revealed no signs of chronic PA obstruction or stricture.
In our study, the mean length of hospital stay in the PAR group was 11.6 days. In the literature, it is reported that the time of hospitalization of patients undergoing PAR is long [1,34]. Although, it was not statistically significant, the duration of hospital stay and duration of intensive care unit stay was found to be higher in PN patients. This may be indicative of physiological disadvantage due to decreased pulmonary reserve after PN.
In our study, hospital mortality was observed in one patient in the PAR group (5%) due to ARDS and sepsis secondary to pneumonia. Although there was no significant difference in mortality between the groups in our study, it has been shown in the literature that parenchymal sparing surgeries could be performed with less mortality rate compared to PN, and the importance of spared pulmonary reserve has been emphasized [12,13,26,34]. Right-sided surgery is the major surgical risk factor in PN [35], however, in our study, most of the patients underwent left pneumonectomy, extended pneumonectomy cases were not included in the study, and the number of the patients in PAR group was low, so we believe that these are the reasons why the mortality rates of PN and PAR groups were similar.
Bronchoplastic procedures have been reported to be an acceptable alternative to PN in terms of survival and local recurrence and have been recommended to be performed whenever possible [10,12,13,24,26]. However, due to the need for complex surgical procedures in angioplasty procedures, the worry that a complete surgery cannot be achieved, and the expectation that local recurrence will increase and thus the survival will decrease, the adaptation of surgeons to this technique has been slow. The number of publications in which long-term survival outcomes of angioplasty procedures have been reported is relatively low in the literature [17-20]. The first 2-year and total 5-year survival results (69% and 59%, respectively) observed in our study are similar to or better than the results of these studies. However, mostly heterogeneous patient populations (tangential resection and original PAR) were analyzed in these studies, and survival results were often presented together with bronchial sleeve resections. Due to the number of patients, demographic characteristics, inclusion criteria, tumor stages, and the differences in the follow-up periods, it is difficult to compare the results obtained in other series with ours and to evaluate the oncological success of our angioplasty practices.
That the arterioplasty concomitant with bronchoplasty is oncologically superior to PN has been demonstrated in some comparative studies [1,19,20,24,26]. It has been reported that it is oncologically successful in the radical local control of the disease and has lower local recurrence rates. In a meta-analysis performed by Ma et al., [21] it was reported that the results of PAR and sleeve lobectomy were similar in terms of postoperative mortality, morbidity, 5-year survival, and local recurrence, and these results were better than PN. Besides, it was reported in that study that PAR application together with sleeve lobectomy is both technically and oncologically as safe as isolated sleeve lobectomy. It was emphasized that radical operations such as PN are not necessary even in higher-stage tumors.
In our study, the first-2-year disease-free survival results (69% and 64% respectively), total 5-year survival results (59% and 56% respectively) and the mean survival time were more advantageous in the PAR group than PN group, but this advantage was not statistically significant. We believe this is because the number of the patients in PAR was low, only the stage I-IIIA tumors were analyzed, and most of the patients in the study had stage II tumors. When the survival results in our study were analyzed according to the intergroup stages, the survival results in early-stage tumors (stage I+II) were found to be similar; however, the survival in PAR group was significantly better than PN group in stage III tumors (52% and 30% respectively). This shows us that even in more advanced stage tumors, more radical operations such as PN are not necessary to achieve a better survival. This may indicate that PN patients, even at the same stage, have a greater central tumor and more lymph node involvement, both of which affect the survival. Besides, no local recurrence was detected on the pulmonary artery suture line or bronchial anastomosis in any of the PAR patients. The possible reasons for this may be that PAR was applied only to the patients with R0, the patients in the study had relatively low stages and the follow-up period was shorter (median 26 months). However, since the majority of lung cancer recurrences occur within the first 2 years [36], it is not possible that our local recurrence rate would have increased dramatically if our follow-up period had been longer.
The main limitations of this study can be listed as follows; its retrospective design, the low number of patients in the PAR group, the heterogeneity in the tumor histology and stages, that the operations were performed by different surgeons, and the short follow-up period.
In conclusion, this study showed that to avoid pneumonectomy in central lung tumors, pulmonary artery reconstructions can safely be performed with acceptable morbidity and mortality rates. According to the comparison between the homogeneous patient groups, oncologic results of pulmonary angioplasty procedures were not worse than those of PN. The PAR group revealed that even in more advanced stage tumors, more radical operations such as PN are not necessary to achieve a better survival. In the light of these data; major anatomical lung resection with pulmonary angioplasty is a suitable procedure not only for patients who cannot tolerate pneumonectomy but also for all patients in whom this procedure is anatomically and oncologically feasible.
Declaration of conflicting interests
The authors declared no conflicts of interest with respect to the authorship and/or publication of this article.
Funding
The authors received no financial support for the research and/or authorship of this article.
Reference
1) Lausberg HF, Graeter, TP, Tscholl D, Wendler O, Schafers HJ. Bronchovascular versus bronchial sleeve resection for lung tumors. Ann Thorac Surg 2005;79:1147-52.
2) Ginsberg RJ. Rubinstein L. For the Lung Cancer Study Group. Randomized trial of lobectomy versus limited resection for patients with T1N0 non small cell lung cancer. Ann.Thorac Surg 1995;60:615-23.
3) Klempnerer J, Ginsberg RJ. Morbidity and mortality after pneumonectomy. Chest Surg Clin N Am 1999;9:512-25.
4) Bernard A, Ferrand L, Hagry O, Benoit L, Cheynel N, Favre JP. Identification of prognostic risk factors determining risk groups for lung resection. Ann Thorac Surg 2000;70:1161-71.
5) Harrison RW, Adams WE, Long ET, Burrows B, Reimann A. The clinical significance of cor pulmonale in the reduction of cardiopulmonary reserve following extensive pulmonary resection. J Thorac Cardiovasc Surg 1958;36:352- 68.
6) Putnam JB, Lammermeier DE, Colon R, McMurtrey MJ, Ali MK, Roth JA. Predicted pulmonary function and survival after pneumonectomy for primary lung cancer. Ann Thorac Surg 1990;49:909-15.
7) Tedder M, Anstadt MP, Tedder SD, Lowe JE. Current morbidity, mortality, and survival after bronchoplastic procedures for malignancy. Ann Thorac Surg 1992;54:387-91.
8) Van Schil PE, Brutel de la Riviere A, Knaepen PJ, van Swieten HA, Defauw JJ, van den Bosch JM. TNM staging and long-term follow-up after sleeve resection for bronchogenic tumors. Ann Thorac Surg 1991;52:1096-101.
9) Tronc F, Gregoire J, Rouleau J, Deslauriers J. Long-term results of sleeve lobectomy for lung cancer. Eur J Cardiothorac Surg 2000;17:550-6.
10) Suen HC, Meyers BF, Guthrie T, Pohl MS, Sundaresan S, Roper CL. Favorable results after sleeve lobectomy or bronchoplasty for bronchial malignancies. Ann Thorac Surg 1999;67:1557- 62.
11) Yoshino I, Yokoyama H, Yano T, Ueda T, Takai E, Mizutani K et al. Comparison of surgical results of lobectomy with bronchoplasty and pneumonectomy for lung cancer. J Surg Oncol 1997;64:32-5.
12) Okada M, Yamagishi H, Satake S, Matsuoka H, Miyamoto Y, Yoshimura M et al. Survival related to lymph node involvement in lung cancer after sleeve lobectomy compared with pneumonectomy. J Thorac Cardiovasc Surg 2000;119:814-9.
13) Deslauriers J, Gregoire J, Jacques LF, Piraux M, Guojin L, Lacasse Y. Sleeve lobectomy versus pneumonectomy for lung cancer: a comparative analysis of survival and sites or recurrences. Ann Thorac Surg 2004;77:1152-6.
14) Shields TW: Lung Cancer: Epidemiology and Carcinogenesis. General Thoracic Surgery, Baltimore, Philadelphia, London: William & Wilkins, ed: TW Shields;2000, Chapter 93, 1215.
15) Yamashita M, Shimizu N, Maruyama S, Ichiba S, Okabe K, Sanao Y et al. Lung cancer operation with pulmonary angioplasty. Jpn J Bronchol 1992;14:123-8.
16) Vogt-Moykopf I, Trainer S, Schirren J. Sleeve lobectomy. Shields TW(Ed): General Thoracic Surgery. Williams&Wilkins, USA, 1994; p.452-60.
17) Rendina EA, Venuta F, De Giacomo T, Ciccone AM, Moretti M, Ruvolo G et al. Sleeve resection and prosthetic reconstruction of the pulmonary artery for lung cancer. Ann Thorac Surg 1999;68:995-1001.
18) Cerfolio RJ, Bryant AS. Surgical techniques and results for partial or circumferential sleeve resection of the pulmonary artery for patients with non-small cell lung cancer. Ann Thorac Surg 2007;83:1971-6.
19) Alifano M, Cusumano G, Strano S, Magdeleinat P, Bobbio A, Giraud F et al. Lobectomy with pulmonary artery resection: morbidity, mortality, and long-term survival. J Thorac Cardiovasc Surg 2009;137:1400-5.
20) Venuta F, Ciccone AM, Anile M, Ibrahim M, De Giacomo T, Coloni GF et al. Reconstruction of the pulmonary artery for lung cancer: longterm results. J Thorac Cardiovasc Surg 2009;138:1185-91.
21) Ma Z, Dong A, Fan J, Cheng H. Does sleeve lobectomy concomitant with or without pulmonary artery reconstruction (double sleeve) have favorable results for non-small cell lung cancer compared with pneumonectomy? A meta-analysis. Eur J Cardiothorac Surg 2007;32:20-8.
22) Nagayasu T, Matsumoto K, Tagawa T, Nakamura A, Yamasaki N, Nanashima A. Factors affecting survival after bronchoplasty and broncho-angioplasty for lung cancer: single institutional review of 147 patients. Eur J Cardiothorac Surg 2006;29:585-90.
23) Chunwei F, Weiji W, Xinguan Z, Qingzen N, Xiangmin J, Qingzhen Z. Evaluations of bronchoplasty and pulmonary artery reconstruction for bronchogenic carcinoma. Eur J Cardiothorac Surg 2003;23:209-13.
24) Martin-Ucar AE, Chaudhuri N, Edwards JG, Waller DA. Can pneumonectomy for non-small cell lung cancer be avoided? An audit of parenchymal sparing lung surgery. Eur J Cardiothorac Surg. 2002; 21:601-5.
25) Kawaguchi T, Tojo T, Kushibe K, Kimura M, Nagta Y, Taniguchi S. Short and long-term outcomes after pneumonectomy for primary lung cancer. Ann Thorac Cardiovasc Surg 2008;14:289-93.
26) Ludwig C, Stoelben E, Stoelben E, Olschewski M, Hasse J. Comparison of morbidity, 30-day mortality, and long-term survival after pneumonectomy and sleeve lobectomy for non-small cell lung carcinoma. Ann Thorac Surg 2005;79:968-73.
27) Suzuki K, Nagai K, Yoshida J, Nishimura M, Takahashi K, Yokose T et al. Conventional clinicopathologic prognostic factors in surgically resected nonsmall cell lung carcinoma. Cancer 1999;86:1976-84.
28) Zieren HU, Müller JM, Hamberger U, Pichlmaier H. Quality of life after surgical therapy of bronchogenic carcinoma. Eur J Cardiothorac Surg 1996;10:223-7.
29) Allison PR: Course of Thoracic surgery, in Groningen. Quoted by: Jones PH. Lobectomy and bronchial anastomosis in the surgery of bronchial carcinorna. Ann R Coll Surg Engl 1959;25:20.
30) Thomas CP. Conservative resection of the bronchial tree. J R Coll Surg Edinb. 1956;1:169.
31) Vogt-Moykopf I. Gefäßplastiken bei Bronchusmanschettenresektion. Prax Klin Pneumol 1974;28:1030.
32) Rendina EA, Giacomo TD, Venuta F, Ciccone AM, Coloni GF. Lung conservation techniques: Bronchial sleeve resection and reconstruction of the pulmonary artery. Semin Surg Oncol 2000;18:165-72.
33) Vogt-Moykopf I, Fritz T, Meyer G, Bu¨lzerbruck H, Daskos G. Bronchoplastic and angioplastic operation in bronchial carcinoma: long-term results of a retrospective analysis from 1973 to 1983. Int Surg 1986;71:211-20.
34) Lausberg HF, Graeter TP, Wendler O, Demertzis S, Ukena D, Schafers HJ. Bronchial and bronchovascular sleeve resection for treatment of central lung tumors. Ann Thorac Surg 2000;70:367-71.



