

2Thoracic Surgery Clinic, Konya Numune State Hospital, Konya, Turkey
3Department of Plastic Reconstructive and Aesthetic Surgery,Selcuk University Medical Faculty, Konya, Turkey DOI : 10.26663/cts.2017.0022
Summary
Pectus excavatum and pectus carinatum are the most common congenital chest wall deformities among others. The current surgical treatment involves insertion of a pectus bar to correct the deformity. It is a minimal invasive technique with minimal incisions but a scar tissue might be seen similar to all surgical interventions. This is an unintended result after surgery. In minimal invasive repairment of pectus deformities, we recommend scar revision after the removal of bar to achieving a good aesthetic outcome.Introduction
Pectus excavatum and pectus carinatum are the chest wall deformities that often require surgical correction for cardiopulmonary and/or especially for cosmetic indications [1,2]. These surgeries are performed via replacing a metal bar to the chest wall by several techniques for the correction of the deformity. However, like all surgical interventions a scar formation might be inevitable. It is a dilemma that a surgery which is performed for cosmetic indications result with a scar formation. We aimed to imply a technique in order to get good aesthetic results after pectus bar surgeries.
Technique
Our suturing technique is performed during the second intervention, i.e. bar removal surgery. In this technique, firstly we excise the scar elliptically, which is formed in the former pectus repair surgery (Figure 1), then remove the bar (Figure 2). After that, we approximate the subcutaneous tissue with 3/0 polyglecaprone sutures in order to reduce dermal tension (Figure 2b) and close the skin with 3/0 polyproplene suture subcutaneously (Fig 2c). Two weeks after the surgery we remove the sutures and start the silicone gel therapy. This scar is considered as the last scar which will not be incised again. Not incising over it but excising the old scar, provides us a more controllable new scar with suture techniques and gels.
 Click Here to Zoom |
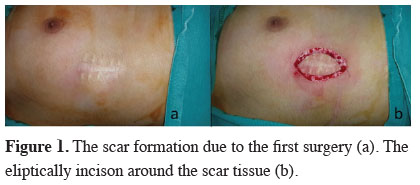
Figure 1: The scar formation due to the first surgery (a). The eliptically incison around the scar tissue (b). |
 Click Here to Zoom |
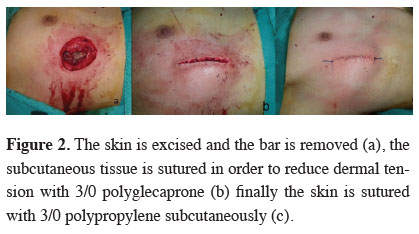
Figure 2: The skin is excised and the bar is removed (a), the subcutaneous tissue is sutured in order to reduce dermal tension with 3/0 polyglecaprone (b) finally the skin is sutured with 3/0 polypropylene subcutaneously (c). |
Discussion
Scar formation is an inevitable result of skin incision in surgery [3]. A satisfactory scar should be flat, narrow and as imperceptable as it can be [4]. If the old scar site will be incised for a second intervention, the last scar would be much worse. Therefore we advise to revise the old scar site in pectus bar removal surgeries.Immature scars tend to give poor results after scar revision [4]. We remove the pectus bar at least 3 years after the first surgery. This time is sufficient for scar maturation. The second surgery gives us enough time to evaluate the scar and the skin quality of the patients. If there is a tendency for a hypertrophic scar or keloid, we could evaluate this condition during the second surgery and after the scar revision, patient will receive an additional medication such as silicone sheets and/or triamcinolone.
Fonkalsrud et al. detected hypertrophic scars in their series and they recommended to use triamcinolone routinely [5,6]. We expanded and developed Fonkalsrud"s technique and added a scar revision and silicone gel application.
Concerning the length of incision during minimal invasive repair of pectus deformities, they are much more favorable than an open surgery. We think that the incision should also be satisfactory after such a minimally invasive procedure, performed for cosmetic reasons. So we recommend this simple but satisfactory scar revision and suturing technique for bar removal surgeries in chest wall deformities.
Declaration of conflicting interests
The authors declared no conflicts of interest with respect to the authorship and/or publication of this article.
Funding
The authors received no financial support.
Reference
1) Frantz FW. Indications and guidelines for pectus excavatum repair. Curr Opin Pediatr 2011; 23: 486-91.
2) Kuru P, Cakiroglu A, Er A, Ozbakir H, Cinel AE, Cangut B, et al. Pectus Excavatum and Pectus Carinatum: Associated Conditions, Family History, and Postoperative Patient Satisfaction. Korean J Thorac Cardiovasc Surg 2016; 49: 29-34.
3) Garg S, Dahiya N, Gupta S. Surgical scar revision: an overview. J Cutan Aesthet Surg 2014; 7: 3-13.
4) Miranda BH, Allan AY, Butler DP, Cussons PD. Scar Revision Surgery: The Patient"s Perspective Arch Plast Surg 2015; 42: 729-34.



